Overview
Osteoarthritis is a common disease affecting the knee. This is because the knee has to take extreme stresses, twists and turns.
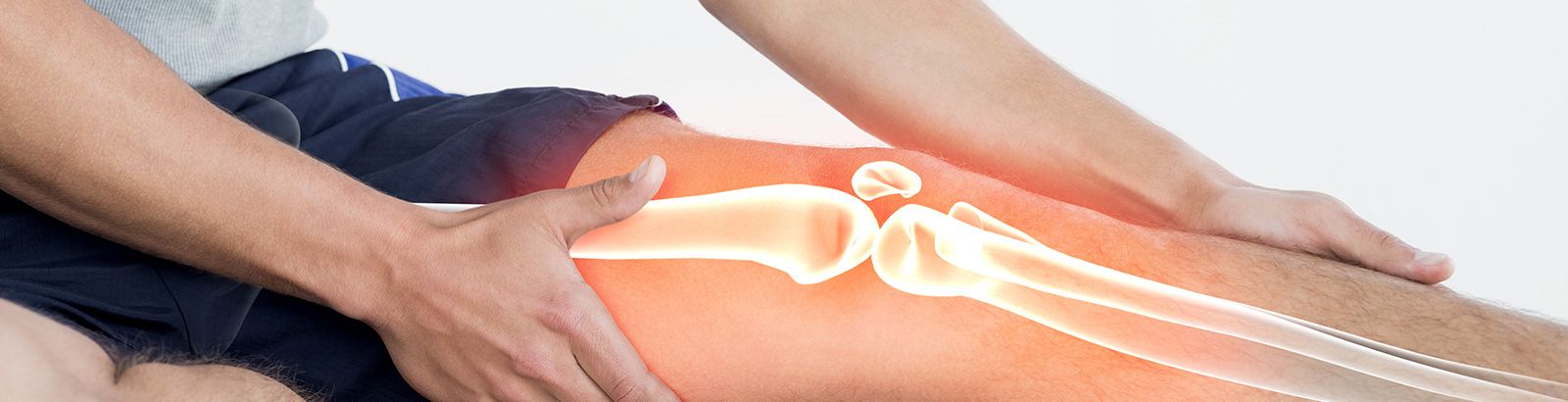
The knee joint is made up of three main bones: your thigh bone (femur), shin bone (tibia) and kneecap (patella). A smooth cartilage layer is found on the bones where they meet and this helps to protect them and give a smooth surface to help movement.
In osteoarthritis, wear and tear can cause this smooth cartilage to gradually roughen and become thinner. This can occur on the main surfaces of the knee joint or underneath your kneecap.
Osteoarthritis of the knee is seen more commonly as you get older, especially over the age of 50 but also as a result of previous injury to the knee.
Symptoms
- Pain – most likely to be felt at the front and sides of your knee. Occurs as this protective cartilage becomes worn out. Worse when standing or moving your joint. Pain felt when resting your joint occurs when osteoarthritis has become severe
- Joint instability – Your knee joint may feel as if it wants to give way when you put weight on it. Legs might become bent or bowed in severe disease.
- Stiffness – occurs due to roughening of the smooth cartilage
- Creaking or grinding (this is called crepitus)
- Swelling (soft or hard)
Symptoms can often be felt to some extent in both knees
Causes
The exact cause of osteoarthritis is not yet understood. Some risk factors have however been identified:
- Age – more common over the age of 50
- Sex – women are more likely to develop osteoarthritis
- Genetics – runs in some families
- Occupation – physically demanding jobs increase wear and tear in the joint
- Weight – being overweight puts more strain on your joints and so increases wear and tear
- Previous injuries – injuries to knee ligaments, cartilage and menisci give a 50% risk of developing osteoarthritis within 5 – 15 years
- Other joint disease – for example gout or rheumatoid arthritis
Treatment
A range of treatments may help to manage your symptoms but will not cure your osteoarthritis. These include:
- Physiotherapy – exercise and strengthening exercises
- Maintaining a healthy weight
- Knee supports and braces
- Painkillers: paracetamol and non-steroidal anti-inflammatory medicines should be used with guidance from your general practitioner or pharmacist
- Injections (i.e. steroids, viscosupplementation, N-stride)
When symptoms can no longer be adequately controlled, partial or total knee replacement surgery can be offered. Cartilage preservation surgery can also be considered for younger patients with higher demands where knee replacements are not advisable.