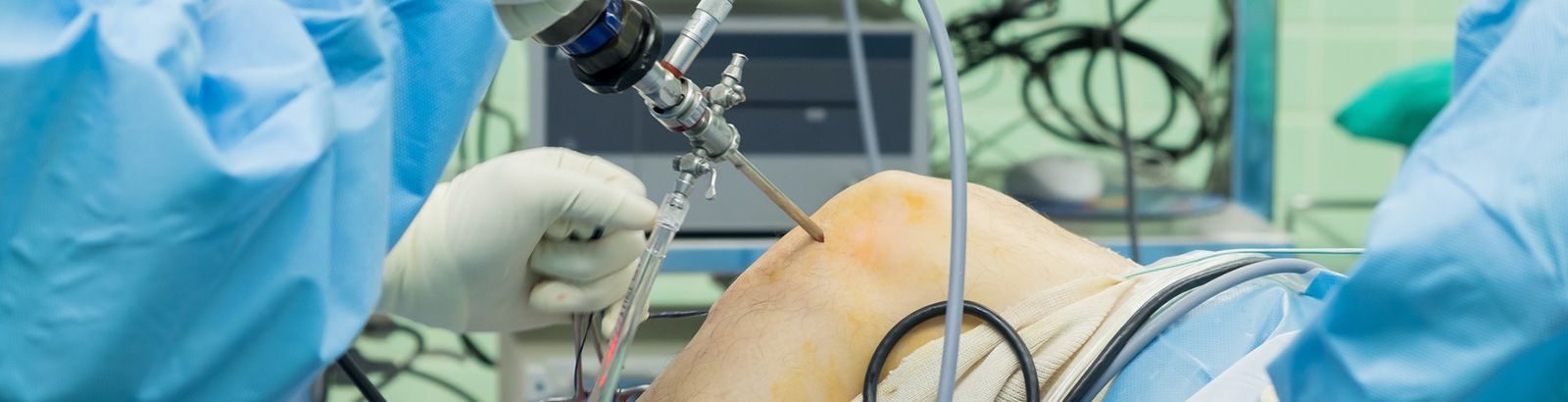
Overview
Ligaments are usually reconstructed rather than repaired as this gives better results.
Reconstruction can use a number of graft choices such as your patellar tendon, hamstrings tendon or a graft from another person (allograft). The choice is usually tailored to your specific problem.
The goals of ligament reconstruction surgery are:
- To restore normal joint anatomy
- Restore knee stability
- Return to work and sport as soon as possible
For this procedure to be a success, it is important that the patient takes an active role in pre and post-operative rehabilitation. Early restoration of full joint movement and weight bearing are very important for successful rehabilitation.
The operation
- This operation is usually done under general anaesthetic
- This operation usually takes between 1 – 2 hours
- A hamstrings or patella tendon graft is harvested through separate incisions in the front of the knee.
- Two or three further incisions are made at the front of your knee for the camera (arthroscope) and other instruments to perform the procedure
- Sterile water (saline) is passed through the knee to make visualisation of the knee structures easier. This fluid is drained at the end of the procedure
- Holes are drilled in the thigh bone (femur) and shin bone (tibia) in order to insert the ligament graft which is then fixed in place with small screws and similar devices
- Local anaesthetic and painkillers are injected into the knee to minimise discomfort after surgery
- Stitches are used to close the wounds and a bandage and temporary splint is applied.
After the operation
- Pain relief – good pain relief is important and you will be given this during your procedure. Some people need more than others so please ask for help if you are in any discomfort following your procedure. You can expect some pain that may last up to a few weeks
- Hospital stay – most patients usually leave the hospital on the same day.
- Physical activities – Full weight bearing can usually be done on the day of your surgery with Physiotherapy guidance.
- Showering and bathing – you need to keep your wound well covered using the waterproof dressing provided whilst showering. When bathing do not submerse wound in water as dressing are not designed to withstand this. This should be done for at least the first 10 days
- Swelling and bruising – Ice: applied for 10-30 minutes at a time. Wrap ice in a plastic bag or towel to prevent ice-burn. Elevation: reduces swelling. Prop up leg using a pillow when sitting or lying in bed. Aim to keep above the level of the heart. Swelling and bruising may take up to 8 weeks to completely disappear.
- You will attend physiotherapy as guided following your operation as part of a pre-arranged rehabilitation programme and it is important to attend all sessions to ensure your surgery is a success.
- Your ability to return to sport will be discussed and decided on by your surgeon and physiotherapist.
Your surgeon and physiotherapist will discuss with you issues surrounding:
- Returning to work
- Using your knee following your operation
- Driving
- Anticipated length of rehabilitation
Possible complications
All surgery has associated risks. These risks are higher in some patients than others. Risks include:
- Anaesthetic – your anaesthetist will discuss risks associated with the anaesthetic with you.
- Infection – there is a small risk of wound or deeper infection following your operation that is minimised by giving you antibiotics. If at any time you notice a fever or increased pain, swelling or redness around you wound, please contact us urgently.
- Nerve or blood vessel damage – this can sometimes occur after surgery and if severe may require a return to theatre.
- Deep vein thrombosis – this is a blood clot in the leg. Rarely, you may be given blood thinning medication and support stocking to help prevent this. If you notice a pain in your calf then please contact us urgently.
- Failure to improve – not all symptoms may be cured by the surgery
- Accidental damage – structures inside or near to the joint may be damaged. This is extremely rare.
- Graft failure and re-rupture – There is an approximately 5% risk that the ACL graft could fail and re-rupture.